Written by Dominic Giuliano
Men’s Health Week provides an important opportunity to discuss critical issues related to the physical and mental health of males across the lifespan.
** CAUTION**
Some readers may find the following information disturbing, as it contains statistics relating to suicide and mental health related issues.
If you or anyone you know is struggling with mental health please contact Lifeline: 13 11 14.
Living in Rural & Regional Areas
People living in rural and regional areas in Australia are presented with distinct mental health challenges.
The combination of
- Geographic Isolation
- Limited access to mental health services
- Socio-economic factors
make it difficult to receive timely and effective treatment.
Many men in these areas face their own unique challenges, and with Men’s Health Week upon us, it’s time to raise the issue.
When it comes to mental health, men are especially susceptible to the pressures of work, economic uncertainty, and social isolation.
While men report lower rates of anxiety and depression in Australia, these statistics may only reflect a reduced ability to recognise, or willingness to report, mental health vulnerability.
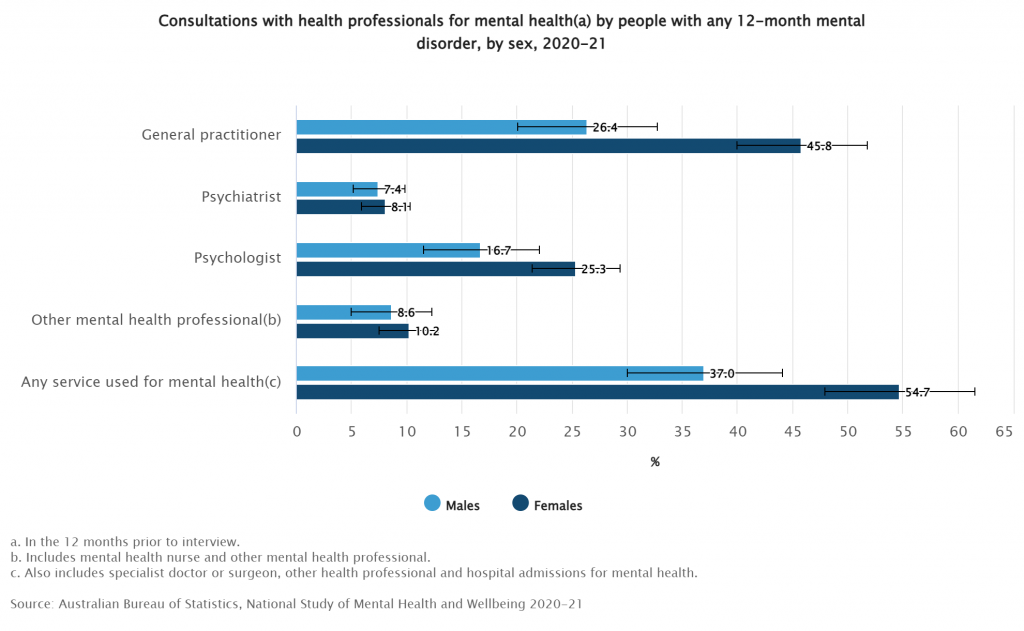
Indeed, data regarding access to professional mental health services between 2020-21 was 1-in-5 for females, but 1-in-8 for males, meaning men are seeking less treatment.
But do men experience fewer or less severe mental health issues?
Australian Masculinity
A key difference may instead come down to how men cope with mental health issues.
We already saw the reduced likelihood for men to request mental health assistance. Furthermore, ABS data reveals higher rates of alcohol and substance abuse among men, and an alarming statistic indicating that 75% of suicides are male.
This persistent trend has spanned at least a century in Australia, with middle-aged males identified as the most vulnerable demographic.
The impact of such poor mental health outcomes on families and communities cannot be underestimated, considering the central role men often play in these contexts.
A significant factor driving this underlying trend is the traditional conception of Australian masculinity.
The stereotypical “Aussie Bloke” is tough, stoic, and independent. Consequently, males who express complaints of illness or depression often face the perception that they are somehow weak or lacking in character.
These stereotypes gain further reinforcement through misinformation regarding available forms of mental health support, particularly psychotherapy.
Seeking help and discussing personal problems may be misconstrued as an inability to handle one’s own issues independently, thus challenging the traditional gender role of a man shouldering burdens independently.
The misguided yet prevailing belief that it is unmanly to share problems with others calls for a paradigm shift, but what can be done?

Creating Change
Change may begin by changing the metaphor of mental health support.
Where seeking mental health support had traditional connotations like “sharing your problems”, “burdening someone else”, or “needing someone’s help”, it may instead be reconstrued as psychological fitness training.
In the same way a personal trainer helps develop strategies for building physical muscle or improving fitness, psychological training is developing strategies for a resilient mind or strengthened relationships. The trainer isn’t needed, but they have expertise in optimising routines for better overall outcomes.
This change in language has fidelity to traditional masculine stereotypes for strength and autonomy and may address some of the stigma surrounding mental health treatment in males.
Other developments such as the proliferation of telehealth and outreach programs may further change what it means to receive treatment.
Likewise, exploring the connection between mental health and behaviour, such as:
- Increasing exercise
- Prioritising sleep hygiene
- Improving dietary habits
- Increasing social interaction
- Engaging in non-occupational hobbies
presents other valuable approaches.
Specifically, encouraging participation in social activities, such as men’s sheds and community events, fosters a sense of belonging and connectedness. These strategies may have the advantage that men often exhibit greater receptiveness to tangible strategies.
Although these solutions provide hope, the challenge of addressing men’s mental health remains a pressing and pervasive issue across Australia.
However, events like Men’s Health Week can play a vital role in changing entrenched beliefs and attitudes some men have concerning their mental well-being.
I was able to find multitudes of information from the National Study of Mental Health and Wellbeing on the ABS Website.











